Hey everybody!
All of us at Airing hope that you and your families are doing well. As well as you can be, that is, during these challenging times. It is difficult enough to suffer from OSA, but with the threat of respiratory distress from this pandemic, please be careful, diligent, and as safe as you can be.
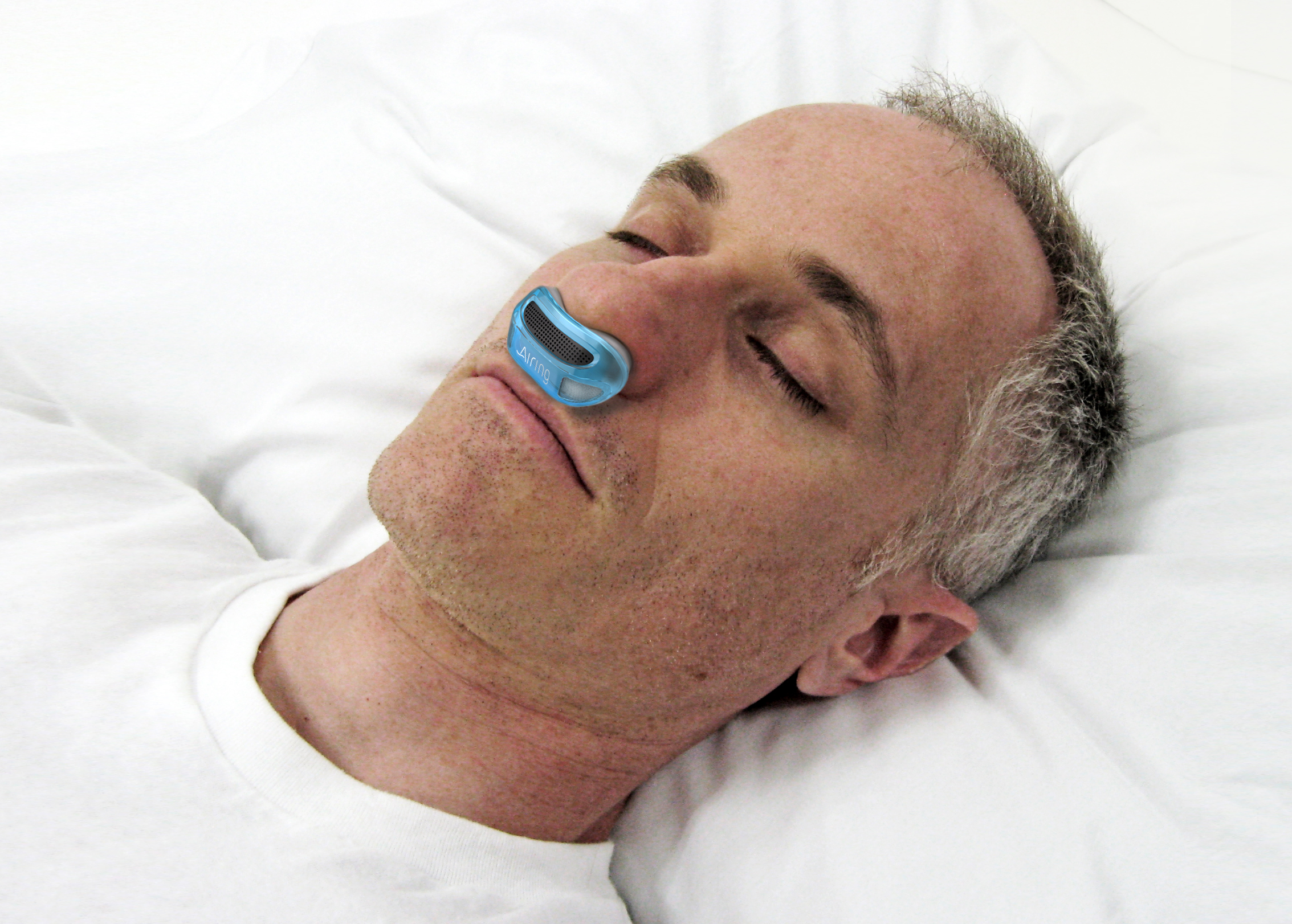
The Airing team has continued working through all of this because we know how important it is to get our micro-CPAP device finished and into the hands of those who so desperately need it. And, we will continue to push as hard as we can to make that happen.
To help us accomplish this goal, we need to hire more scientists and engineers. So, we are reaching out to our community, that means you, to see if any of you have the expertise and desire to join our mission. We have added an Employment tab (www.fundairing.com/employment) to our website.
There, you can find a description of the positions we need to fill. If you are interested and you believe you have the expertise we are looking for, please let us know by sending your resume to hiring@fundairing.com. A bigger team will help us accelerate the development process. If it is not you, please let your friends and colleagues know about this opportunity. It would be wonderful to fill these positions with one of you!
Again, we are working hard to get the micro-CPAP product finished and out to you all as soon as possible. But, until then, please try and use your CPAP machine if you have stopped, because with the COVID-19 virus out there, it is even more important now that you stay as healthy as you can!
Best,
The Airing Team